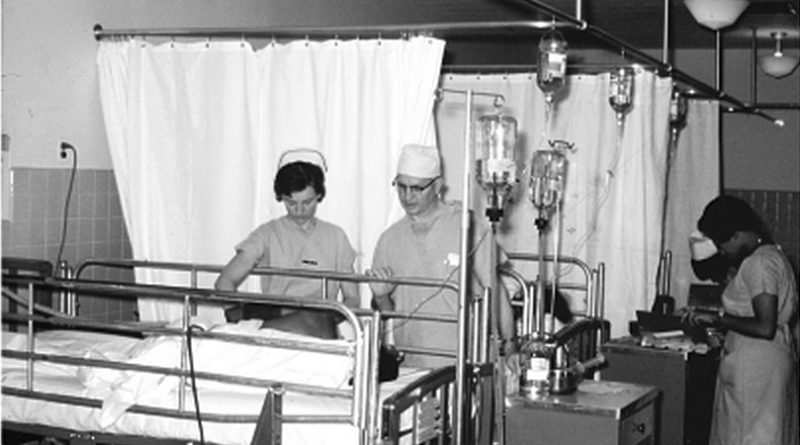
Hughes Springs, Texas native ‘Dr. Pepper’
Above photo, Dr. Marion ‘Pepper’ Jenkins and nurses administering a crystalloid solution at Parkland Memorial Hospital of Dallas around 1960. Dr. Jenkins pioneered the use of saline solutions for trauma and surgery patients in 1950.
From The East Texas Journal, May 2013
JFK assassination overshadowed contribution of practicing physician who pioneered anesthesiology

The fame brought about from the Kennedy assassination “became a burden. He did not want to get involved in conspiracy theory debates,” said Dr. Marion “Pepper” Jenkins’ daughter, Christine L. Jenkins.
In terms of the history of medicine, Hughes Springs-born Dr. Jenkins, is a footnote. In terms of the universal impact of his use of Ringer’s Lactate saline solutions for trauma and surgery patients, his work is used daily.
The achievements of the doctor from Hughes Springs are publicly overshadowed by his attempt to resuscitate President John F. Kennedy. Fame followed him from the attempt to save the one life, while his innovation for trauma and surgery patients has saved millions of lives the world over and revolutionized how anesthesiology is administered since 1950.
Born into a family of medicine, Marion “Pepper” Jenkins came from humble beginnings in the small town of Hughes Springs. Pepper was the second son of Homer Jenkins, a country doctor who was noted to have worked well into his seventies delivering babies, riding horseback from neighbor to neighbor, according to Brynda Hennings in a note on findagrave.com. Five of Pepper’s six brothers also became doctors, as well as three of his foster brothers, seven of his eight uncles, and his two sons. His eighth uncle became a pharmacist.
Completing his Bachelor of Arts degree by age 20, Pepper continued on to complete his medical degree at the University of Texas Medical Branch at Galveston in 1940. Moving to Kansas City, Pepper met and married his wife of 53 years, Elizabeth “Betty” Weaver, while working a rotating internship at the University of Kansas Hospital from 1940-1941. Moving back to Galveston, Pepper assumed an Assistant Residency in Internal Medicine at John Sealy Hospital.
World War II drew young Dr. Jenkins to active service in the US Navy in the South Pacific from 1942-1946. His four years of war service aboard the USS Chandeleur during the battles of Guadalcanal and Kwajalein shaped an interest in improving the treatment of the traumatized wounded marines. Treating the injured during the war was lieutenant commander Jenkin’s first experience with anesthesia.
Upon moving back to Texas to focus on internal medicine, Pepper began a residency at Parkland Memorial Hospital because of an established reputation for excellence in the management of civilian trauma. His mentors, Dr. Carl Moyer and Dr William Lee Hudson urged Pepper to specialize in anesthesiology, according to Dr. Phillip Montgomery. They wanted Pepper to start a new teaching department at Parkland Memorial and Southwestern medical School.
“Pepper wanted to go into surgery, and Moyer told him he wasn’t going to let him… he was going to send him to Boston to learn anesthesiology,” said Dr. Montgomery.
“So Pepper said, ‘Yes sir,’ and went.”
After one year of residency in anesthesiology at the Massachusetts General Hospital, Pepper returned to Dallas to a position of Director of the Department of Anesthesiology at Parkland Hospital and Parkland Memorial Hospital, serving from 1948 until 1981. The division of anesthesiology, founded by Pepper in 1948, became a separate department from the department of surgery in 1955.
In January of 1949, Pepper established the first hospital recovery room west of the Mississippi River. He saw to desegregating the surgical and waiting rooms the same year, according to Surgery: The First Fifty Years, a history of the University of Texas Southwestern Medical Center at Dallas.
In 1950, Drs Jenkins, Carl Moyer, Tom Shires, and Ben Wilson presented “a revolutionary proposal to use balanced salt solutions in the treatment of surgical and traumatic shock; one of the most important innovations in the modern care of the surgical patient,” Epoch of Fluid Therapy and Trauma by Wilson William.
“This discovery is comparable to the revelation that the Earth orbits the sun,” said Dr. Ed Johnson, Chairman of the anesthesiology department of UT Southwestern Medical.
Dr. Carl Moyer established a prevalent understanding with physicians that a traumatized patient was intolerant to salt. In Moyer’s experiments, “he gave a liter of normal saline to a series of healthy medical students and observed that all the sodium was promptly excreted in the urine. The balance of sodium intake and output was perfectly maintained in the healthy human body. The same salt load was given to anesthetized surgical patients, but they did not excrete the sodium,” said Wilson William. The kidneys, because of the anesthesia and trauma, retained the salt load. Moyer’s conclusion was “that the patients were intolerant to the sodium and recommended that salt be withheld from anesthetized surgical patients,” said William. He presented this research in October 1946 at the Massachusetts General Hospital centennial of the introduction of anesthesia.
Moyer’s conclusions were widely supported by influential and established physiologists, resulting in patients receiving transfusions of whole blood, with no added electrolytes. Complications arose in critical patients in hemorrhagic shock who received whole blood transfusions developed “high hematocrits, stiff lungs, and pulmonary failure… a condition named ‘congestive atelectasis’,” according to the team of doctors, which could be “prevented if patents were given simultaneously a fluid that resembled extracellular fluid (in those days, Ringer’s lactate).”
At the same time, Dr. Tom Shires was performing experiments with these fluids in hemorrhagic shock in dogs and humans. His work “validated the use of balanced salt solutions in hemorrhagic shock,” said William. “Salt solutions were no longer felt to be contraindicated in surgical patients. Instead they were indicated and, in fact, were life-saving. Our concepts of fluid therapy in traumatized patients were thereafter changed forever.”
Moyer admitted his error. Jenkins applauded his actions saying “it seems quite appropriate to praise a remarkable man, Carl A. Moyer, as a giant among physicians and a leader of great integrity. It must not have been easy for him to reverse published opinions for which he received considerable acclaim”.
“The use of balanced salt solutions in the resuscitation of traumatic, hypovolemic shock has been accepted all over the world and has saved millions of lives. The revolutionary proposal in 1950 by Dr. Pepper Jenkins and his colleagues to give salt solutions to surgical patients changed forever the way we practice medicine and the way we think about fluid therapy in the surgical patient,” said William.
Dr. Jenkins provided testimony on March 11, 1963 for the Warren Commission, an investigation into the assassination of President John F. Kennedy. Arlen Specter was council of the President’s Commission who interviewed Dr. Jenkins.
Noon on November 22, 1963, Dr. Pepper Jenkins received an unusual STAT emergency call while in the dining room of Parkland Hospital. A second STAT in succession signaled him to move quickly. Dr. Ronald Jones called in about the STAT, stating with a colorless, anguished face, “The President has been shot and is on his way to the hospital.”
At that moment the sirens could be heard as the ambulance sirens pulled in to the driveway on Harry Hines Boulevard.
“I ran up the stairs to the Anesthesia Department, that’s on the second floor-one floor above the dining room, where I was, and notified two members of the Department, the first two I saw, my Chief Associate, Dr. &. H. Giesecke, Jr., and Dr. Jackie Hunt, that the President had been shot and was being brought to the emergency room and for them to bring all the resuscitative equipment we have including an anesthesia machine. The emergency room is set up well, but we are used to working with our own equipment and I asked them to bring it down and I ran down the back stairs, two flights down, and I arrived in the emergency room just after or right behind him being wheeled in, I guess,” said Jenkins in his testimony about the incident to Arlen Specter.
From his World War II trauma experience, Jenkins “was aware of what he was in an agonal state” with a “respiratory gasp made up of jerking movements. His eyes were opened and somewhat exophthalmic (protruding) and color was a greatly suffused, catanotic-purplish cyanosis,” reported Jenkins in his testimony. “Still, we have patients in that state, as far as cyanosis and agonal type respiration, who are resuscitatable. Of course you don’t stop at this time and think, ‘Well, this is a hopeless circumstance,’ because one in this state can often be resuscitated. This represents the activities prior to one’s demise sometimes, and if it can be stopped, such as the patient is oxygenated again and circulation reinstituted, he can be saved,” he said.
“I felt no peripheral pulse and was not aware of any pulse. I reported this to Dr. Kemp Clark and he started closed chest cardiac massage,” said Jenkins. “at this time I was aware of the magnitude of the wound, because with each compression of the chest, there was a great rush of blood from the skull wound,” said Jenkins.
President Kennedy was pronounced dead at exactly 1300, according to Dr. Jenkins’ watch. “I think, as we pronounced the President dead, those in attendance who were there just sort of melted away. Well, I guess ‘melted’ is the wrong word; but we felt like we were intruders and left,” said Jenkins.
In regards to the time of death, “for a period of minutes, but I can’t define exactly, since I didn’t put this in a report, after we knew he was dead, we continued attempting resuscitative maneuvers. When we saw the two priests who arrived in the corridor outside the emergency room where this was taking place, I went to the door and asked one of those men what is the proper time to declare one dead. That is, I am not a Catholic and I was not sure of the time for the last rites. As I remember now, he said, ‘The time that the soul leaves the body is not at exactly the time that medical testimony might say that death was declared.’ There would be a period of time, and so if we wished to declare him dead at that time, they would still have the final rites.”
“This was a very personal-on the part of the very anguished occasion; and Mrs. Kennedy had come back into the room and most of the people were beginning to leave because they felt like this was such a grief stricken and private affair that they should not be there,” said Jenkins.
Dr. Jenkins continues in his testimonies to describe the head wound as a point of exit, as well as a wound on the neck as a second point of exit. This enforces the famous two-bullet theory insinuating a second gunman.
Dr. Marion Jenkins was also on duty, catching up on paperwork, when Kennedy’s assassin, Lee Harvey Oswald was brought in after being shot by Jack Ruby. Oswald was fatally wounded at 11:21am on November 24, 1963 as he was being transferred to the Dallas County Jail. This shooting occurred on live television.
Jack Ruby was convicted of murder in 1964 and sentenced to death. The judgment of death was reversed in 1966. Ruby was treated by Dr. Jenkins for galloping lung cancer but died on January 3, 1967, before his second trial could begin.
Dr. Jenkins was awarded seven distinguished service awards for medicine. In 1988, he became the first anesthesiologist to win the American Medical Association’s Distinguished Service Award, one of the most prestigious honors in medicine, reported the Dallas Morning News in Jenkins’ obituary.
On October 13 of this year, Washington DC will see the gathering of the 17th Annual meeting of the Pepper Jenkins Society Alumni, where students who received their training from Dr Jenkins meet to honor his memory. Dr. Marion “Pepper” Jenkins died from stomach cancer on November 21, 1994, ironically, a day shy of the 31st anniversary of John F. Kennedy’s assassination in Dallas.